Articles
On completing 100 days in office, Yogi Adityanath, the Chief Minister of Uttar Pradesh (UP), reaffirmed his government’s commitment to a major revamp of the healthcare sector in the state. Accordingly, the state health ministry is trying to overcome the multiple challenges of shortage of doctors and poor healthcare infrastructure. The government is seeking to upgrade the existing hospitals and overcome a shortage of 7000 doctors and 18000 paramedical staffs. This process, if completed, would be a welcome change in the most populous state in the country, which has been devoid of affordable, accessible and quality healthcare for decades. The state battles daunting health challenges – incompetent and insufficient healthcare centres, staff, medicines and medical equipment.
A brief study of the basic health infrastructure and basic health indicators like the Infant Mortality Rate (IMR) and Maternal Mortality Rate (MMR) illustrates the bleak condition of healthcare in UP. In 2005, UP was one of the eight states identified as the Empowered Action Group (EAG) states based on their dismal health indicators. Data from the Annual Health Survey (AHS) 2012–13 reveal that UP continues to be one of the poorest performing states, lagging behind the national average on most of these indicators.
Inadequate Healthcare Infrastructure
The Sub Centres (SCs), Primary Health Centres (PHCs) and Community Health Centres (CHCs) are the various interfaces of the government’s healthcare system. These centres at various levels are supposed to provide affordable and quality healthcare accessible to all. According to the Census 2011, 22.27 per cent of the state’s population lived in urban areas and 77.73 per cent of the state’s population lived in rural areas. However, the state has only one PHC per 28 villages or 44597 people.
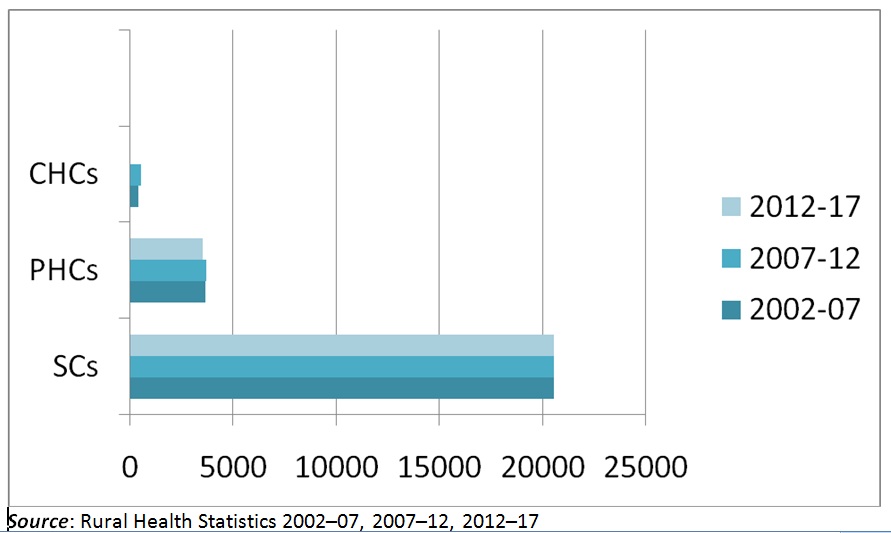
Over the decades, the number of health centres in the state has increased only marginally. Even though the number of CHCs has increased from 515 in the period 2007–12 to 773 in 2012–17, the growth appears trivial, when the huge population of the state is taken into account.
Graph 1: Number of PHCs, CHCs and SCs in UP in the period 2002–17
PHCs and CHCs are inadequately staffed and together account for only half the combined strength of staff. Considering that UP contributes to 16.6 per cent of the country’s population, it has only 10.81 per cent of health workers. According to the Rural Health Statistics 2016, CHCs in UP reported a shortage of 84 per cent of specialists. In terms of density of nurses, most of the 30 districts with the lowest numbers were located in UP, followed by Bihar and Jharkhand. According to a World Health Organisation (WHO) study of 2016, UP has the lowest share of female health workers of 19.9 per cent, compared with the Indian average of 38 per cent.
Infant Mortality Rate
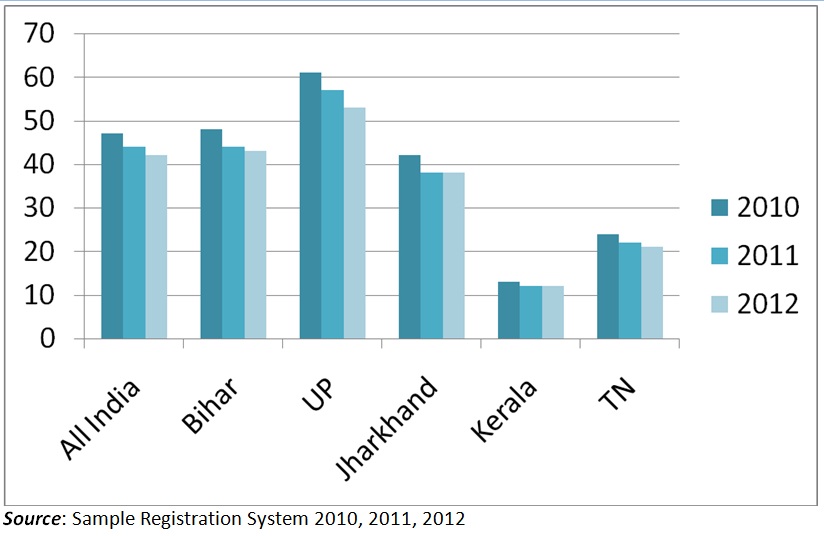
Data from Rural Health Statistics 2015 reveal that UP has the second highest IMR (deaths per 1000 live births) across rural and urban areas in the country. Over the decades, UP has recorded higher IMR across genders than the national average. A newborn in UP is expected to live four years fewer than in the neighbouring state of Bihar, five years fewer than in Haryana and seven years fewer than in Himachal Pradesh.
Graph 2: Comparison of IMR across States in the Period 2010–12
Maternal Mortality Rate
The state also accounts for the second highest MMR in the country with 285 maternal deaths for every 100,000 live births. UP has the highest child mortality indicator, from the Neonatal Mortality Rate (NNMR) to the less-than-five mortality rate.
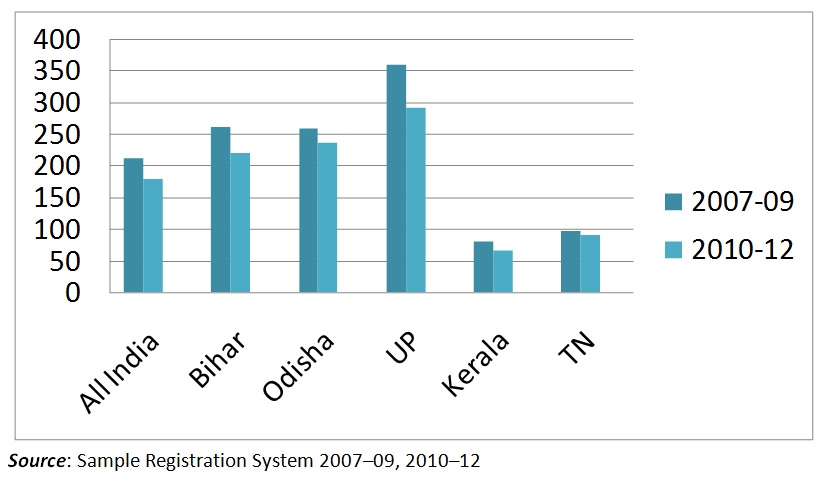
Although the MMR dropped from 212 deaths in 2007–09 to 178 deaths in 2010–12, India is lagging behind the target of 103 deaths per 100,000 live births, which was to be achieved by 2015 under the United Nations-mandated Millennium Development Goals (MDG).
Graph 3: Comparison of MMR across States in the Period 2007–12
Diseases and Deaths
UP contributed to the largest share of deaths, due to communicable and non-communicable diseases, including 48 per cent of typhoid deaths (2014), 17 per cent of cancer deaths and 18 per cent of tuberculosis deaths (2015).
In 2016, of the total number of 1277 Acute Encephalitis Syndrome (AES) cases reported in India, 615 were reported in UP. The state also accounts for more than 75 per cent of Japanese Encephalitis (JE) cases. Of the total number of 275 deaths due to JE, 73 were reported in UP.
The dismal performance of the state’s healthcare sector has continued unabated over the last few decades. Evidently, the successive governments in the state have failed to provide quality healthcare to the people. One major reason can be the below-par expenditure on health by the state. UP spends an average of 4.7 per cent of its social sector expenditure on public healthcare and family welfare annually. This is marginally less than the national average of 4.8 per cent.
In October 2016, the Allahabad High Court observed that healthcare in UP was worsening by the day and that the state governments have failed to deliver. The incumbent UP government, which has alleged that it has inherited ‘a completely broken system’, has its task cut out. To begin with, the Adityanath government has emphasised on maximum use of technology in healthcare and upgrading the state’s healthcare network from basic PHCs to multispecialty hospitals. Also for the first time, the UP government is planning to develop a state-specific health policy, which would cater to its unique health challenges. It is high time the state realised that quality healthcare is not a privilege but a fundamental right.
*Anupama Ghosh is Research Intern, CPPR
Views expressed in this article are personal and do not reflect those of CPPR.
Dr Anupama Ghosh is Senior Research Associate and the Internship Co-ordinator at CPPR. She holds a PhD in History from the University of Delhi. She can be contacted by email at [email protected] and on twitter @anupama86ghosh